|
In this study 60 patients with a functional gait disorder were randomised to a 3-week inpatient physical rehabilitation programme or a 4-week waiting list. 
The first controlled trial of physical-based rehabilitation for FMD, published in 2014, compared an intervention group with patients waiting for treatment. A number of cohort studies report positive results from physical interventions that are based on a biopsychosocial understanding of FMD and encompass psychosocial therapeutic elements. In recent years, specialist physiotherapy has emerged as a promising treatment for FMD. 
However, little is known about the outcome of patients who receive timely specialist interventions. A systematic review of long term follow up studies found that approximately 40% of patients were the same or worse at an average of 7 years and the majority of patients remained symptomatic. The long-term outcome is variable but often poor. The incidence of FMD is reported to be in the range of 4 to 12 per 100,000, making it similar in incidence to multiple sclerosis and Parkinson’s disease. FMD is often described as a condition at the interface between neurology and psychiatry. It is also common for patients with FMD to have comorbid health problems such as neurological disease. 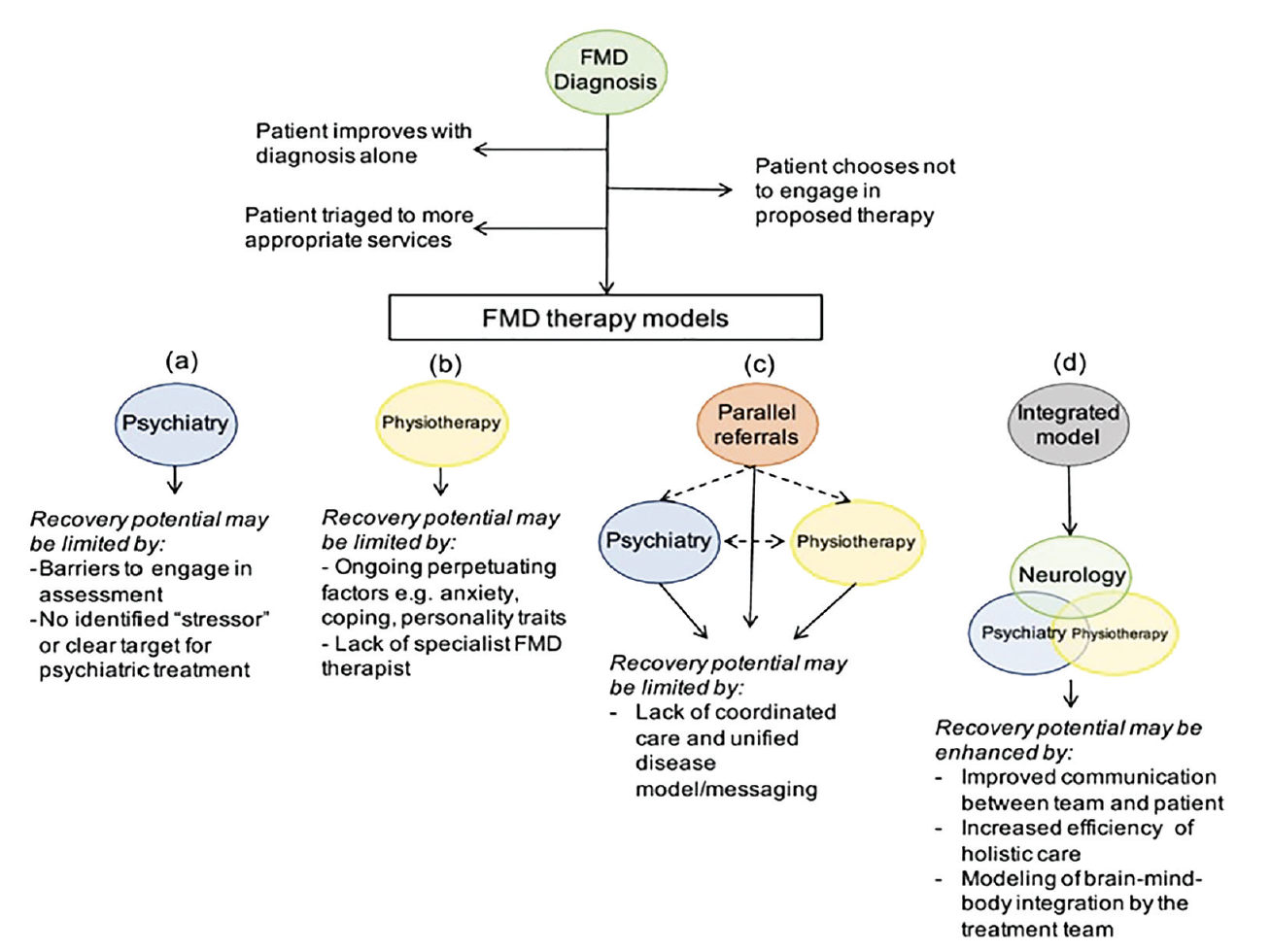
Most patients also experience non-motor functional neurological symptoms, such as sensory disturbance, memory complaints, pain, fatigue or dissociative seizures. Typical presentations of FMD include weakness, tremor, jerks, dystonia, gait disorder, or a combination of these symptoms. FMD is the motor-dominant variant of functional neurological disorder (also known as conversion disorder). Registered 27 March 2018.įunctional motor disorder (FMD) can be defined as neurological symptoms affecting movement that are caused by loss of control or agency over movement, rather than a structural disease process. International Standard Randomised Controlled Trials Number ISRCTN56136713. This trial will be the first adequately-powered RCT of physical-based rehabilitation for FMD. Health economic analysis will evaluate the cost impact of trial and control interventions from a health and social care perspective as well as societal perspective. Secondary domains of measurement will include participant perception of change, mobility, health-related quality of life, health service utilisation, anxiety and depression. The primary outcome is the Physical Function domain of the Short Form 36 questionnaire at 12 months. Participants will be followed up at 6 and 12 months. 264 Adults with a clinically definite diagnosis of FMD will be recruited from neurology clinics and randomised to receive either the trial intervention (a specialist physiotherapy protocol) or treatment as usual control (referral to a community physiotherapy service suitable for people with neurological symptoms). The trial is a pragmatic, multicentre, single blind parallel arm randomised controlled trial (RCT). 
Here we present the protocol of a randomised controlled trial (RCT) that aims to evaluate the clinical and cost effectiveness of a specialist physiotherapy programme for FMD. Physiotherapy is usually considered an important part of treatment however, sufficiently-powered controlled studies are lacking. Patients with functional motor disorder (FMD) experience persistent and disabling neurological symptoms such as weakness, tremor, dystonia and disordered gait.
0 Comments
Leave a Reply. |

 RSS Feed
RSS Feed
